A Practical Guide to Medical Billing Denial Management
When a claim gets denied, it’s not just a piece of paper you have to deal with later. It’s a direct hit to your practice’s bottom line. For any healthcare provider, the process of investigating, appealing, and finally resolving these denials is what we call denial management. Done right, it's how you recover revenue that would otherwise be lost for good.
Think of it this way: a solid denial management strategy isn't just about chasing old claims; it's about protecting the financial health of your entire practice.
The Real Cost of Unchecked Claim Denials

Claim denials feel like an administrative headache, but they’re much more than that. They are a quiet but escalating threat to your practice’s financial stability. For small or specialty clinics, where consistent cash flow is everything, the impact of even a small increase in denials can be devastating. Every denial is another chip taken out of your revenue, creating a ripple effect of financial and operational issues that are tough to climb out of.
And it’s not getting any easier out there. Looking ahead to 2025, providers are seeing a sharp rise in claim denials. In fact, over 41% of providers are now reporting denial rates topping 10%, a big jump from just a few years ago. This trend is getting worse thanks to persistent staffing shortages and technology that just can’t keep up, creating a perfect storm for revenue leakage.
The Direct and Hidden Costs
The most obvious cost is the money you don't get for the service you provided. But the true financial damage runs much, much deeper. The direct cost to rework a single denied claim can be anywhere from $25 to over $118 once you account for your staff’s time and effort. That's money spent whether you win the appeal or not.
Beyond that, a high denial rate quietly drains your practice in other ways:
- Lost Staff Productivity: Your team gets bogged down chasing paperwork, waiting on hold with payers, and drafting appeal letters instead of focusing on patient care and other tasks that actually generate revenue.
- Tanking Team Morale: There’s nothing more frustrating for a biller than fighting with payers all day, only to see the same denials pop up again and again. It leads directly to burnout and high turnover.
- Crippled Cash Flow: Denials stop your revenue cycle in its tracks. The longer a claim festers in accounts receivable, the less likely you are to ever see that money, making it harder to pay bills, order supplies, and grow your practice.
The real kicker? It’s not just the cost of fighting denials. It’s the staggering 65% of denied claims that are never even resubmitted. That’s pure, unrecoverable revenue walking right out the door.
Why Proactive Denial Management is Urgent
For specialty practices—think cardiology, oncology, or mental health—the stakes are even higher. These fields live and die by complex coding, multi-step procedures, and rigid prior authorization rules, making them prime targets for denials. A single denied claim for a high-value procedure can throw off an entire month's revenue projections.
This is exactly why you can't afford to be reactive anymore. Shifting to a proactive denial management strategy isn't just a good idea; it's an absolute necessity for survival. When you focus on preventing denials before they happen, you’re not just plugging holes in your revenue stream. You’re freeing up your team to focus on what matters most: your patients.
Understanding the full picture here is a key part of effective revenue cycle management. This guide is your playbook for making that critical shift—turning denial management from a frustrating cost center into a powerful strategic advantage.
Decoding the Root Causes of Your Denials

To really win the fight against denials, you have to start thinking like a detective. Every single denial code tells a story, pointing to a specific breakdown somewhere in your revenue cycle. The trick to solid denial management isn't just working the denial—it's learning to translate those cryptic codes into real intelligence that shows you exactly which process needs fixing.
Think of it this way: a denial isn't a final "no." It's feedback from the payer. The goal is to shift from just reacting to individual rejections to proactively identifying the systemic issues causing them in the first place. That mindset is what separates practices that are always struggling from those that are financially stable.
The Most Common Culprits Behind Denials
While the reasons can feel endless, most denials fall into a few key categories. Knowing these buckets helps your team diagnose problems faster and focus their energy where it will actually make a difference.
-
Front-End and Registration Errors: These are often the easiest to prevent, yet they remain a top source of denials. A simple typo in a patient's name, an incorrect date of birth, or an expired insurance ID can get a claim kicked back instantly. It all comes down to data accuracy from the very first touchpoint.
-
Authorization and Eligibility Issues: This is a huge pain point, especially for specialty practices. A denial for "services not authorized" means a critical step was missed long before the patient was ever seen. It could be a failure to get a prior auth or just a simple mistake in verifying active coverage for that specific service.
-
Coding and Documentation Gaps: Here, the problem is with the clinical and billing info on the claim itself. This could be an incorrect CPT or ICD-10 code, a missing modifier (which is crucial for things like telehealth), or clinical notes that don't adequately prove the medical necessity of the service.
The financial bleed from these issues is no joke. One in 5 claims gets rejected on the first submission, and a shocking 35% of those are never pursued. This is preventable revenue just walking out the door, and it hits small practices the hardest. The good news? Up to 76% of denials come from these kinds of fixable, process-related issues. You can get more details on prevention in this in-depth report on StatMedical.net.
We see this all the time with telehealth. A practice correctly bills for a virtual visit but forgets to add the '95' modifier to indicate it was done via telehealth. The payer’s system, not seeing a physical place of service, automatically denies the claim. The root cause isn't some complex clinical error—it's a simple, avoidable coding oversight.
A Practical Reference for Diagnosing Root Causes
Connecting a denial code to its real source is the first step toward a permanent fix. To make this easier, your team needs a quick-reference guide that cuts through the jargon and points to a specific workflow breakdown.
The table below provides a clear link between common denial codes you see every day and the real-world problems that cause them.
Common Denial Codes and Their Root Causes
| Denial Reason Code (Example) | Common Root Cause | Preventive Action |
|---|---|---|
| CO 22 – This care may be covered by another payer per coordination of benefits. | Front-Desk Workflow Failure. The patient’s primary and secondary insurance information was not correctly verified or updated at check-in. | Implement a mandatory, real-time eligibility check for every patient at every visit. Train front-desk staff to ask specific questions about changes in insurance coverage. |
| CO 50 – These are not covered services because this is not deemed a ‘medical necessity’ by the payer. | Clinical Documentation Gap. The provider’s notes did not sufficiently justify why the service was necessary for the patient’s diagnosis or condition. | Conduct regular training for clinical staff on payer-specific documentation requirements. Use EHR templates that prompt for medical necessity details. |
| CO 18 – Duplicate Claim/Service. | Billing Process Error. The same service was billed twice, or the claim was resubmitted before the original had fully processed. | Establish a clear “days to wait” policy before resubmitting a claim. Use your clearinghouse reports to track claim status in real time to avoid accidental duplicates. |
| PR 197 – Precertification/authorization/notification absent. | Prior Authorization Process Breakdown. The administrative team failed to secure the required authorization before the service was performed. | Create a centralized prior authorization tracking system or log. Assign clear responsibility for obtaining and documenting authorization numbers before patient appointments. |
By categorizing and analyzing your denials this way, you stop playing whack-a-mole with claims. You start fixing the broken processes that cause denials in the first place, building a much more resilient and profitable revenue cycle.
Building Your Proactive Denial Prevention Playbook
Let’s be honest: great denial management isn’t about being a world-class appeals writer. It’s about making appeals a rare event.
The single biggest shift any practice can make for its financial health is moving from reactive "fire-fighting" to proactive prevention. This playbook is all about building rock-solid front-end processes that stop denials before a claim even exists.
Believe it or not, a staggering 76% of denials come from simple, preventable errors made on the front end. This means your best defense is a strong offense, one that starts the moment a patient schedules an appointment. When you get it right from the beginning, a huge source of financial stress turns into a stable, predictable system.
The Pre-Submission Claim Audit Checklist
Think of a pre-submission audit as your claim’s final quality check. It's a systematic review designed to catch the common mistakes that trigger instant rejections from payers. For a small practice, this doesn't have to be some drawn-out, bureaucratic process. It should be a simple but powerful checklist your team uses every single day.
This checklist is your first line of defense. Here’s what it absolutely must include:
- Patient Demographics Verification: Does the name, date of birth, and policy number on your claim exactly match what the insurance company has on file? A single typo or an old address is all it takes to get a denial.
- Real-Time Insurance Eligibility: You have to confirm active coverage for the specific date of service. An insurance card isn't enough; your team needs to use an electronic tool to verify the policy is active and actually covers the services you're providing.
- Prior Authorization Confirmation: If an auth was required, is a valid authorization number clearly documented? If you don't have one, that claim is almost guaranteed to be denied. It’s a non-starter.
- Code and Modifier Accuracy: Do the CPT and ICD-10 codes tell a clear and accurate story about the visit? Are you using the right modifiers for things like telehealth or bilateral procedures? These small details make a big difference.
Leveraging Your Clearinghouse for Early Warnings
Your clearinghouse isn't just a digital mailbox—it's one of your most powerful diagnostic tools. Most clearinghouses generate rejection reports that flag errors before a claim even makes it to the payer. These aren't technically denials; they're rejections you can fix and resubmit right away, often on the same day.
Treat your clearinghouse rejection report as a daily to-do list. These rejections are free intelligence, telling you exactly what needs to be fixed. Ignoring them is like ignoring a warning light on your car's dashboard; the problem will only get worse and more expensive down the road.
Make reviewing these reports a non-negotiable part of your daily workflow. Start looking for patterns. If you keep seeing rejections for invalid policy numbers from one specific payer, you know you have a training issue at the front desk that needs to be addressed.
Automating Eligibility for Maximum Impact
Checking insurance eligibility manually for every patient is a recipe for burnout and mistakes. This is where automation is a small practice's best friend.
Setting up automated, real-time eligibility checks through your practice management system is a game-changer. Most modern systems can run batch checks on all scheduled patients a day or two in advance. This gives your staff a clean list of anyone with coverage problems, giving them time to sort it out before the patient even walks in the door. It's a foundational part of a strong mental health eligibility and benefits workflow and is just as vital for every other specialty.
The Foundational Role of Credentialing
Finally, we have to talk about one of the most overlooked—yet most fundamental—parts of denial prevention: provider credentialing. If a provider isn't properly credentialed and enrolled with a payer, every single claim you submit for them will be denied. Period. These are the most frustrating denials because the clinical care was perfect, but the administrative paperwork was flawed.
Maintaining solid credentialing files isn't a one-time thing. It’s an ongoing process that involves:
- Proactive Re-credentialing: Keeping a close eye on expiration dates for medical licenses, DEA registrations, and board certifications so there are never any gaps.
- Accurate Payer Enrollment: Making sure every provider is correctly linked to the practice’s tax ID and physical location in every single payer system.
- Timely Updates: Immediately notifying payers of any changes, like a new office address or a provider leaving the practice.
When you weave these proactive steps into your daily operations, you completely change the game. You stop chasing lost money and start protecting your revenue from the very beginning, building a much more resilient and profitable practice in the process.
A Smart Framework for Managing and Appealing Denials
Even with the best prevention playbook, some claim denials are going to happen. It's just a reality of the business. When a denial lands on your desk, your response is what separates recovered revenue from a permanent write-off.
The key is to stop the chaotic scramble. You need a structured, systematic framework that turns medical billing denial management into a predictable, even profitable, process.
Without a system, it's human nature for billers to grab the newest denials or the ones that seem easiest to fix. That isn't always the smartest approach. A well-defined workflow ensures your team’s limited time is spent on claims with the highest chance of a successful appeal and the best return on that time investment.
Triage and Prioritize Your Denials for Maximum ROI
Let's be clear: not all denials are created equal. Trying to tackle every single one with the same level of urgency is a fast track to burnout and lost revenue. A simple triage system helps you focus your efforts where they’ll actually move the needle.
You should categorize every incoming denial into priority levels based on a few key factors:
- Dollar Amount: High-value claims always get immediate attention. A single successful appeal on a large claim can be more impactful than winning ten smaller ones.
- Reason Code and Complexity: Group denials by their root cause. Simple fixes, like a claim denied for a missing modifier, can be resolved in minutes. Medical necessity denials, on the other hand, require a much more intensive, evidence-based appeal.
- Filing Deadlines: Every payer has a strict window for submitting appeals. Your triage process absolutely must flag claims with approaching deadlines to prevent them from being lost to a technicality.
Of course, the best way to manage denials is to stop them from happening in the first place. This simple, three-step prevention process should be your first line of defense, dramatically cutting down the number of denials that even require triage.
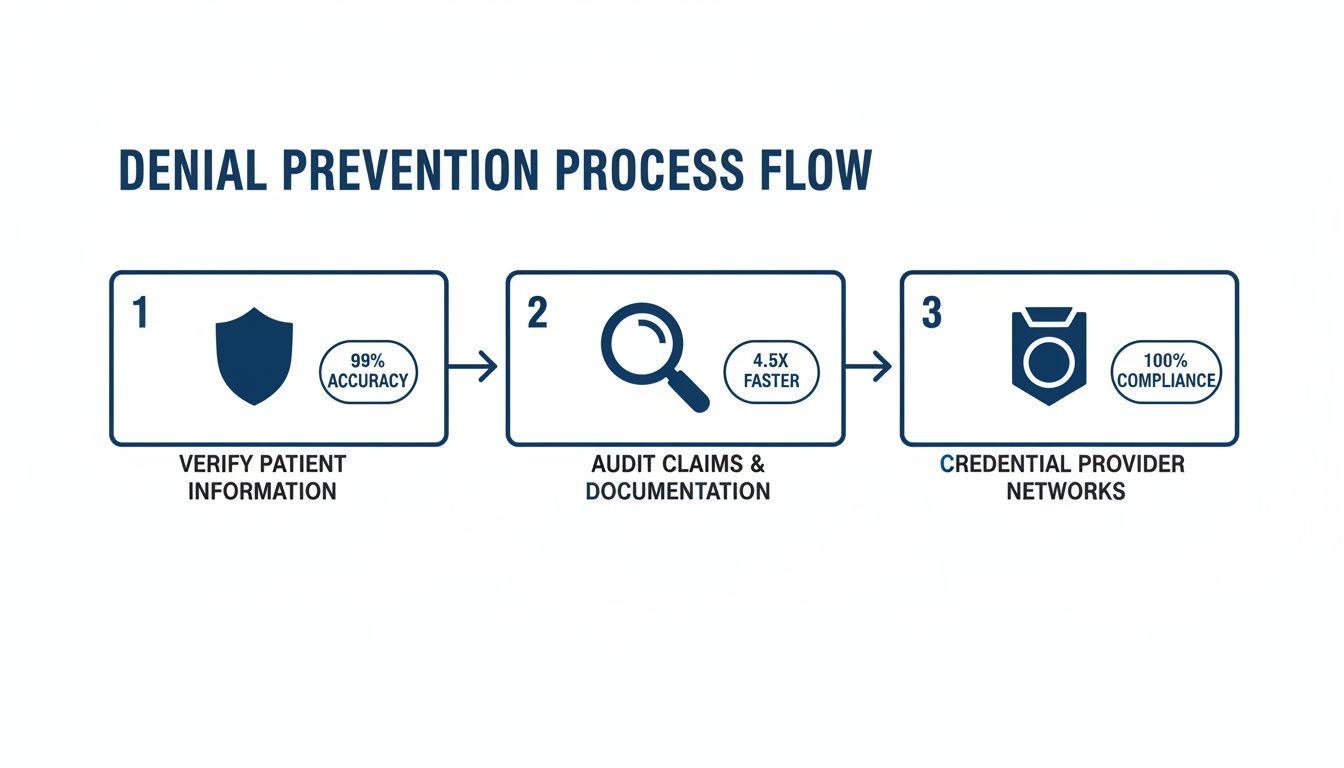
By consistently verifying eligibility, auditing claims before submission, and keeping provider credentials up to date, you eliminate the most common—and most frustrating—sources of denials.
To make this practical, here’s a matrix you can adapt to guide your team's daily workflow. It helps turn abstract priorities into concrete first steps.
Denial Triage and Prioritization Matrix
| Priority Level | Denial Characteristics (Dollar Value, Reason) | Recommended First Action | Typical Turnaround Time |
|---|---|---|---|
| High | High-dollar claims ($1,000+) approaching filing deadline (within 30 days). Complex medical necessity or authorization issues. | Immediate review by a senior biller. Gather all clinical documentation and start drafting the appeal letter. | 2-5 business days to appeal |
| Medium | Mid-range dollar claims with common coding errors (e.g., wrong modifier, invalid diagnosis code). | Assign to a biller for a corrected claim submission. If resubmission is not an option, prepare a simple appeal with corrected info. | 24-48 hours to correct/appeal |
| Low | Low-dollar claims ($50 or less) with simple administrative denials (e.g., demographic error, timely filing). | Batch-process these fixes. Correct data entry errors and resubmit claims in bulk. Make a quick call if needed. | < 24 hours to correct |
This matrix isn't set in stone. Adjust the dollar values and timelines to fit your practice's specific situation, but the core idea remains: focus your best efforts on your biggest opportunities.
Crafting a Compelling and Evidence-Based Appeal
Once you've prioritized a denial, the next step is building an appeal that is clear, concise, and frankly, impossible for the payer to ignore. A strong appeal isn't an emotional plea; it's a professional, evidence-based argument that systematically dismantles the payer's reason for the denial.
Here’s how to structure your appeal letter for maximum impact:
- Start with the Basics: Clearly state the patient's name, policy number, date of service, and the original claim number. Make it brain-dead simple for the reviewer to find everything.
- State the Reason for the Appeal: Get straight to the point in one sentence. For example, "We are appealing this denial for CPT code 99214, which was incorrectly denied as not medically necessary." No fluff.
- Present Your Evidence: This is the heart of your appeal. Reference specific clinical notes, lab results, or imaging reports that justify the service. The pro move? Cite the payer’s own medical policies to show exactly how the care you provided aligns with their published guidelines.
- Maintain a Professional Tone: Keep the language factual and respectful. Frustrated or accusatory language only works against you. You’re presenting a logical case that a reviewer can easily approve.
A common mistake I see is simply resubmitting the claim with a note attached. This almost never works. A formal appeal letter, complete with supporting medical records and a clear argument, shows the payer you're serious and have built a strong case for reimbursement.
Tracking and Following Up on Every Appeal
Submitting the appeal is only half the battle. If you don't track its status, it can easily vanish into the black hole of the payer's system. Meticulous tracking is a non-negotiable part of this process.
Create a simple log or use your practice management software to monitor every single appeal you send out.
Your log should include the date the appeal was sent, the payer's expected response time (check their provider manual), and a calendar reminder for follow-up. If you haven't heard back by that date, a polite but firm phone call is your next move. This consistent follow-up ensures your appeals get the attention they deserve and dramatically increases your chances of getting paid.
Using KPIs and Technology to Sharpen Your Strategy

If you aren't measuring your denial management efforts, you can't improve them. A modern denial management strategy runs on data, not guesswork. Key Performance Indicators (KPIs) are the vital signs of your revenue cycle, giving you objective feedback on what’s working and what’s broken.
Tracking these numbers shifts your entire approach from reactive to strategic. Instead of wondering why cash flow is tight this month, you can pinpoint the exact source of revenue leakage and take targeted action. This data-driven mindset is what separates struggling practices from financially resilient ones.
Essential KPIs for Denial Management
To get a clear picture of your practice's financial health, you need to monitor a handful of critical metrics—consistently. These KPIs provide the insights you need to make smarter, faster decisions.
Here are the non-negotiable metrics to get on your dashboard:
- Clean Claim Rate (CCR): This is the percentage of claims accepted by a payer on the first submission. A high CCR (you should be aiming for 95% or higher) tells you that your front-end processes are solid. If this rate starts to dip, it's an early warning that something is wrong with your pre-submission checks.
- Denial Rate: This one is straightforward—it’s the percentage of claims denied by payers. While the industry average is creeping toward 10%, a well-managed practice should target a denial rate of 5% or less. The real power comes from tracking this by payer and reason code, which tells you exactly where to focus your prevention efforts.
- Net Collection Rate (NCR): This KPI shows how much of your allowed reimbursement you are actually collecting. It’s a direct measure of your billing team's effectiveness. A healthy NCR should be in the high 90s, proving you are successfully collecting the money you've earned.
Monitoring your Days in Accounts Receivable (A/R) is also crucial. This metric tracks the average number of days it takes to collect payments. A rising A/R is a clear signal that denials are creating a cash flow bottleneck and require immediate attention.
The Role of Automation and AI in Modern RCM
Manual processes simply can't keep up with the complexity of modern medical billing. Today's automation and Artificial Intelligence (AI) tools are genuine game-changers, especially for small or specialty practices with lean teams. These technologies handle repetitive, time-consuming tasks with a speed and accuracy that humans can't match.
For example, AI-driven predictive analytics can analyze claims before submission, flagging those with a high risk of denial based on historical data and specific payer behavior. This allows your team to intervene proactively, correcting potential errors before they ever leave your system.
The growth here is significant. The global healthcare denial management market was valued at $14.98 billion and is projected to grow substantially, largely fueled by new regulations demanding better data sharing to curb rejections. As practices fight back against rising denial rates, investing in smarter systems is becoming essential for survival. You can explore more about these trends in this detailed market analysis.
Practical Tech for a Smarter Workflow
Getting started with technology doesn't have to be a massive, overwhelming overhaul. You can begin with targeted tools that solve your biggest headaches first.
- Automated Status Checks: Instead of your staff spending hours on hold with insurance companies, automated systems can check the status of outstanding claims electronically and deliver real-time updates.
- Intelligent Claim Scrubbing: Before a claim goes out the door, software can "scrub" it for common errors—like invalid codes, missing information, or modifier issues—and alert your team to make corrections.
- Digital Appeal Management: Modern platforms can help auto-generate appeal letters using pre-approved templates, attach the necessary documentation, and track the appeal all the way through to resolution.
By combining sharp KPI monitoring with smart technology, you create a powerful feedback loop. The data from your KPIs tells you where the problems are, and the technology gives you the tools to fix them efficiently. This cycle of continuous refinement is the core of a successful and sustainable medical billing denial management strategy and a vital part of your overall accounts receivable management strategy.
Got Questions? Let's Talk Denial Management
Even with a killer strategy, you're going to have questions. Denial management is a moving target. Here are some of the most common ones I hear from practice managers and providers, along with some straight-up advice.
What Is a Good Claim Denial Rate for a Specialty Practice?
The industry average is creeping toward 10%, but don't let that be your benchmark. A well-run specialty practice should be aiming for 5% or less. Honestly, the best ones I’ve worked with consistently hit 2-4%. It’s not a fantasy number; it’s achievable with the right systems.
But here’s the real secret: the static number isn't the whole story. The trend is what matters. If your denial rate is slowly ticking up—even if it's still under that 5% mark—that's your warning sign. It’s a canary in the coal mine telling you a process is breaking down somewhere. You have to track this monthly. It’s non-negotiable for financial health.
How Can a Small Practice Improve Denial Management with a Lean Staff?
If you're a small practice with a lean team, you have to live by the 80/20 rule. Don't try to solve everything at once; you'll burn out your staff.
Start by running one simple report: your top five to ten denial reasons from the last 90 days. I guarantee a handful of recurring issues are causing the vast majority of your headaches. Focus all your energy on preventing just those issues.
For example, is "missing prior authorization" your number one problem? The single most effective thing you can do is create a mandatory pre-visit verification checklist for your front desk. It's a targeted fix that delivers a huge financial impact without overwhelming your team. Small wins build momentum.
When Should We Consider Outsourcing Our Denial Management?
Outsourcing stops being an "if" and becomes a "when" once you see a few persistent warning signs. If your denial rate is stuck above 7-10% no matter what you try internally, that’s a clear signal your team is underwater.
Another big tell is when your staff is bogged down in complex appeals or your days in A/R just keep climbing month after month. That’s not just a billing problem; it's an operational bottleneck that’s costing you real money.
You also need to look at your tech stack. If you can't easily track denial trends or keep up with constantly changing payer rules, a dedicated revenue cycle partner brings the expertise and infrastructure you're missing. The ROI shows up fast:
- A lower overall denial rate because experts are preventing them and fighting them.
- Faster payments and a serious drop in your days in A/R.
- Less administrative drag on your team, freeing them up for patient-facing work.
Ultimately, you outsource when the cost of lost revenue and staff burnout is higher than the investment in a partner who lives and breathes this stuff. It's about shifting resources to get a better financial outcome.
At ClaiMed Solutions, we don’t just manage denials—we turn them into a source of revenue intelligence. Our TrustedRCM Method™ uses proactive claim audits and real-time analytics to help our partners achieve a 98-100% collection rate. Stop chasing lost cash. Start protecting it from day one. Schedule your complimentary, zero-stress strategy call today and see what's really possible.
Powered by the Outrank app