How to Improve Medical Billing Process and Boost Cash Flow
It can feel like you're fighting a losing battle against rising claim denials and slow payments, but the answer isn’t a massive, disruptive system overhaul. The truth is, you can dramatically improve your medical billing process with smart, strategic adjustments to your existing workflow. By focusing on pre-submission audits, coding accuracy, and proactive denial management, you can boost your clean claim rate and get cash in the door much faster.
Charting Your Path to Financial Health
A healthy revenue cycle is the lifeblood of a thriving medical practice. Yet, so many practices get bogged down by the sheer complexity of it all. From the first moment a patient registers to the final payment, the billing process is a journey full of potential pitfalls where tiny errors snowball into significant financial setbacks.
The goal here isn't to work harder; it's to work smarter. By taking a structured approach, you can systematically plug the leaks in your revenue cycle and build a resilient financial foundation for your practice. This is about putting practical, field-tested concepts to work—like a 'ClaimShield Protocol' designed to catch errors before they ever leave your office and a 'ClearView Dashboard' that gives you real-time financial insights.
The High Cost of Inefficiency
The financial stakes have never been higher. Recent data shows that medical billing denial rates have climbed to a staggering 11.8%, a noticeable jump from 10.2% just a couple of years ago. With nearly 38% of organizations reporting denial rates of 10% or more, billions in earned revenue are being left on the table every year.
This trend hits independent specialty practices the hardest, where high-value, complex claims are often the first to get denied. But there's good news: achieving a high clean claim rate—the percentage of claims paid on the very first submission—is entirely within your reach. While the industry benchmark is 95% or better, I’ve seen countless practices boost their rates from the low 80s to over 96%. The result? They slash their days in accounts receivable (A/R) by an average of 15 days. You can find more detail on these industry challenges and solutions.
Key Takeaway: Just imagine getting paid two full weeks faster on every single claim. That’s the real-world impact of optimizing your billing process. It translates directly into cash you can use for staffing, new equipment, or expanding your practice.
A Multi-Layered Strategy for Success
To really improve your medical billing process, you need a multi-layered approach that shores up every single touchpoint in the revenue cycle. This isn't about fixing one thing; it's about creating robust systems for everything that matters.
This means putting solid processes in place for:
- Pre-Submission Audits: A final quality check to verify codes, patient data, and payer-specific rules before a claim goes out the door.
- Coding and Documentation: Ensuring clinical notes fully support the services billed and that codes are applied with precision.
- Streamlined Claim Submission: Using the right tools and best practices to transmit clean claims efficiently every time.
- Proactive Denial Management: Building a system to quickly analyze, appeal, and learn from every denial to stop it from happening again.
The infographic below illustrates this strategic flow perfectly. It starts with protective pre-submission checks, moves to clear financial oversight, and ultimately leads to sustainable growth.
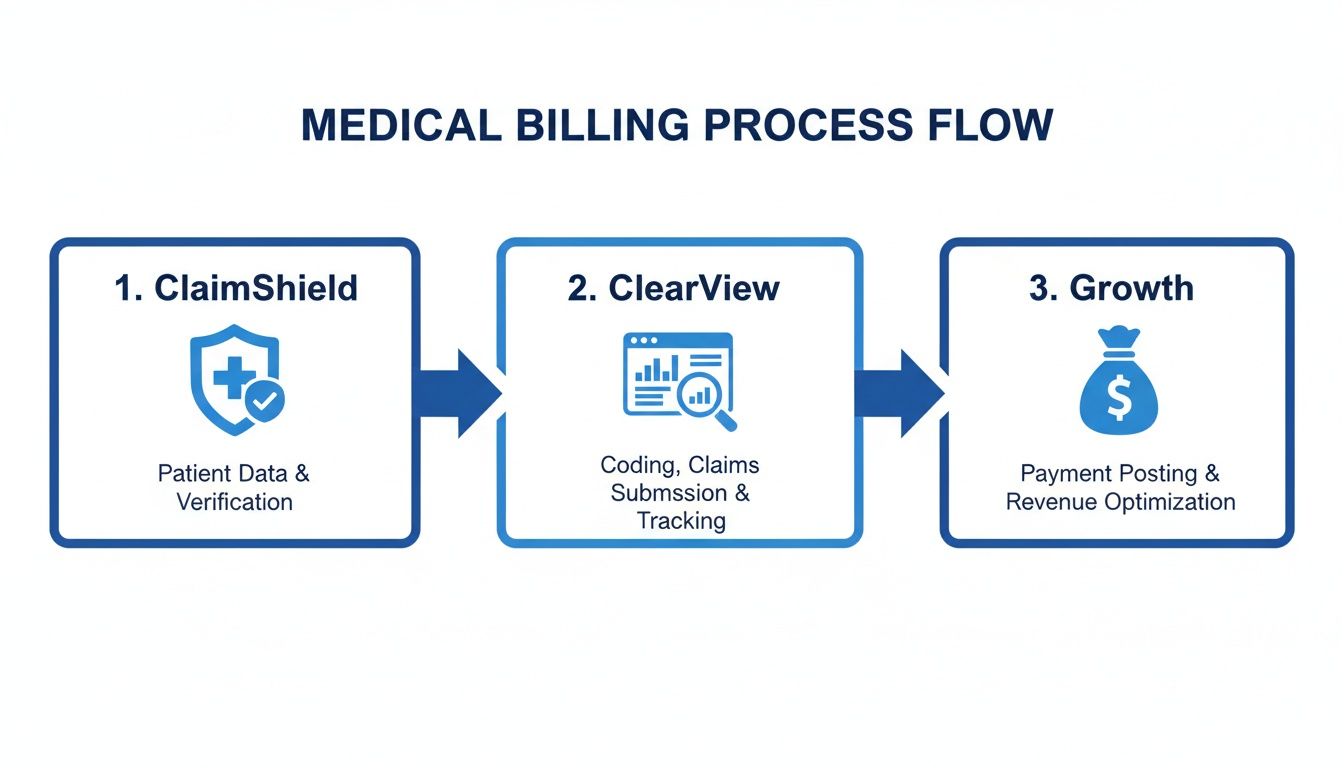
This visual roadmap shows how a 'ClaimShield' protocol acts as the foundation. This leads directly to the 'ClearView' dashboard for tracking performance, which results in measurable financial growth for your practice.
To put it simply, a truly optimized workflow isn’t a series of disconnected tasks but a cohesive system where each stage supports the next.
Key Stages of an Optimized Medical Billing Workflow
| Stage | Primary Goal | Key Action |
|---|---|---|
| Patient Registration & Verification | Ensure 100% accuracy from the start. | Verify eligibility, benefits, and demographics before every visit. |
| Charge Capture & Coding | Bill for all services rendered, accurately. | Use code scrubbers and review documentation to match services. |
| Pre-Submission Audit | Achieve a >95% clean claim rate. | Implement a final quality check for errors before submission. |
| Claim Submission & Tracking | Get claims to payers quickly and monitor status. | Submit claims electronically within 24-48 hours of service. |
| Payment Posting & Reconciliation | Post all payments accurately and identify issues. | Reconcile ERAs against expected allowables to catch underpayments. |
| Denial Management & Appeals | Recover revenue from denied claims. | Analyze denial reasons, appeal promptly, and fix root causes. |
| A/R Follow-Up & Collections | Keep aging accounts to a minimum. | Systematically work outstanding claims based on age and value. |
| Reporting & Analytics | Gain visibility into financial performance. | Use dashboards to track KPIs like denial rate, clean claim rate, and days in A/R. |
Each stage is a critical link in the chain. When they all work together seamlessly, you move from a reactive, frustrating process to a proactive, predictable revenue engine.
Strengthening Your Front-End Patient Intake Process
Some of the most powerful improvements you can make to your medical billing happen long before a provider walks into the exam room. It’s a hard truth, but a staggering number of claim denials come from simple, preventable mistakes made right at the front desk.
Think about it. A single typo in a patient’s name, an old insurance policy number, or a missed prior authorization can bring a claim to a screeching halt.

These aren't complex coding errors; they're cracks in the foundation of your patient intake workflow. When you start treating your front desk as the first line of defense for your revenue cycle, you can wipe out a huge portion of common denials and watch your clean claim rate climb. This proactive stance sets the entire billing journey up for success.
Implement Real-Time Insurance Eligibility Verification
Finding out a patient's insurance is inactive after they've been seen is a recipe for lost revenue. The fix? Make real-time eligibility and benefits verification a non-negotiable step for every single appointment. This goes for new patients and established ones alike.
Modern practice management systems can—and should—automate this. The best setups run a check when the appointment is scheduled and then again 24-48 hours before the visit. This simple step confirms active coverage and, just as importantly, clarifies the patient's financial responsibility.
Your front-desk team needs to be trained to look for four key things:
- Active Policy Status: Is the coverage actually in effect today?
- Copay, Coinsurance, and Deductible: What, exactly, will the patient owe out-of-pocket?
- Coverage Limitations: Are there any services that their plan simply won't cover?
- Prior Authorization Requirements: Does the planned service need a green light from the payer beforehand?
Catching an eligibility problem before the visit gives your team the power to solve it. They can collect updated insurance info on the spot or, if needed, reschedule the appointment until the coverage is sorted out.
Develop and Communicate a Clear Financial Policy
Confusion is the enemy of timely payment. Patients often put off paying bills because they genuinely don't understand what they owe or why. A clear, concise, and easy-to-read financial policy is your best tool for setting expectations from day one.
This document should be written in plain language, not healthcare jargon. Every new patient should get a copy during intake, and you should have established patients review it annually. The policy needs to spell out when payment is due, what payment methods you accept, and what happens if a balance goes unpaid.
Pro Tip: Don't just slide a form across the counter and ask for a signature. Coach your staff to spend 30 seconds walking new patients through the key points, like paying their copay at the time of service. This tiny bit of engagement prevents massive billing headaches down the line.
This is especially critical for a specialty practice like orthopedics, where procedures can get expensive. Providing a good-faith estimate based on verified benefits turns a potentially awkward money conversation into a moment of transparency and trust. It’s a cornerstone of any strategy to improve your medical billing process.
Master the Prior Authorization Workflow
For many specialties, prior authorization is the single biggest administrative nightmare. Failing to secure pre-approval is one of the most common—and most costly—reasons for high-dollar claim denials. Your practice needs a bulletproof system to manage this beast.
First, create a master list of the services and procedures that most frequently require authorization from your top 5-10 payers. This helps your team get ahead of the game.
Next, assign clear ownership. One person or a small, dedicated team should be responsible for submitting requests, following up relentlessly, and communicating the approval status to the clinical team and the patient. Using software to track these requests is a game-changer. It prevents things from falling through the cracks and ensures you get paid for the critical care you provide.
Ensuring Coding Accuracy for Clean Claim Submissions
After a patient leaves your office, their visit has to be translated into the language of insurance payers. This is where clinical care becomes a payable claim, and it's arguably the most critical junction in the entire billing process. Getting this translation right is what separates practices with healthy cash flow from those constantly chasing down denials.
The goal isn't just to pick a code; it's to ensure every single code is鉄olidly backed by the clinical documentation. Think of it as building a case for reimbursement so airtight that a payer has no logical reason to deny it. While modern coding software does a great job of scrubbing claims for obvious errors, it's the human oversight that catches the nuanced mistakes.

Mastering Modifiers for Specialty Care
This is where things often go sideways, especially for specialty practices. Modifiers, those little two-digit codes, provide essential context. They explain how a service was altered, and using them correctly—or forgetting them entirely—is often the difference between getting paid and getting a denial.
A chiropractor, for example, absolutely needs to use modifier AT (Acute Treatment) on a spinal manipulation claim to tell Medicare the service is medically necessary, not just maintenance care. Miss that tiny detail, and the claim is dead on arrival.
It's the same story in mental health. A therapist who provides an individual session (90834) and a family session (90847) on the same day must use a modifier like 59 to show they were separate and distinct services. Without it, the payer assumes it's a duplicate charge.
Key Takeaway: Think of modifiers as the grammar of medical coding. Without them, your billing sentences don't make sense to payers, leading to confusion and denials. Regular training on payer-specific modifier rules is essential.
Implementing a ClaimShield Protocol
To truly bulletproof your billing, you need a final quality check before any claim goes out the door. We call this a ClaimShield Protocol. It’s a human-led, pre-submission audit designed to catch the subtle errors that software misses and push your first-pass resolution rate (FPRR) to 95% or higher.
This isn't just another checklist. It's a focused review that zeroes in on three core areas:
- Code Verification: Do the ICD-10 codes truly justify the CPT codes billed? Is the E/M service level fully supported by the provider's notes? This is all about establishing undeniable medical necessity.
- Bundling and Unbundling: The review cross-references claims against National Correct Coding Initiative (NCCI) edits. This confirms you aren't unbundling services that belong together or, just as importantly, forgetting a modifier when two procedures are legitimately performed separately.
- Payer-Specific Rules: Does this claim meet the unique, often quirky, requirements of the patient's specific insurance plan? A commercial payer might have a rule about a certain procedure that’s completely different from Medicare’s.
For practices looking to really sharpen their skills here, exploring specialized medical coding services can offer an expert perspective.
This final checkpoint is your last, best chance to turn a risky claim into a clean one. Adopting this protocol is a proactive move that directly boosts cash flow by slashing the time your team spends on rework and appeals. It gets them off the phone chasing old mistakes and frees them up to focus on growing the practice. The goal is simple: get it right the first time.
Mastering Denial Management and AR Follow-Up
Look, even if you nail every single front-end task and submit perfect claims, some denials are just going to happen. It's a fact of life in this business. The real difference between a practice that's financially stable and one that's always scrambling is how they handle those denials.
The goal isn't just to overturn one rejection. It's to use the data from that denial to stop the next ten before they even start. This is a big shift—moving away from a simple "appeal and forget" mindset to a system that analyzes, corrects, and actually improves your entire process.

Categorize Denials to Uncover Root Causes
Your first move is to stop looking at denials as one giant, overwhelming pile. Start sorting every single one by its root cause. This simple act turns a chaotic mess into data you can actually use.
Group your denials into a few common buckets:
- Registration and Eligibility Errors: This is all front-desk stuff—incorrect patient info, inactive insurance, or coordination of benefits mix-ups. A spike here tells you exactly where you need to retrain.
- Missing or Invalid Prior Authorization: This is a huge one, especially for specialty practices. It’s almost always a sign that communication broke down before the patient was ever seen.
- Coding Errors: Think incorrect CPT or ICD-10 codes, forgotten modifiers, or bundling issues. These problems point straight to a need for more coder training or better provider documentation.
- Medical Necessity: This is when the payer claims the service wasn't clinically appropriate. These denials are tougher and usually require a detailed appeal with rock-solid supporting documentation.
When you track these trends, you create a powerful feedback loop. Seeing a jump in eligibility denials? It's time to get the front desk back on track with real-time insurance verification.
Adopt a Prioritized AR Follow-Up Plan
Not all outstanding claims are created equal, and your team's time is precious. A smart Accounts Receivable (AR) follow-up strategy doesn't just mean working down a list. It means focusing your energy on the accounts that will actually impact your cash flow.
I’ve found the most effective approach is to segment your AR aging report into priority tiers:
- High-Dollar, New Denials (0-30 days): These are your crown jewels. They're the most valuable and the most winnable claims. Jump on them immediately while the details are fresh and you're nowhere near the appeal deadlines.
- High-Dollar, Aging Claims (60+ days): These are flashing red lights. They need immediate escalation because they represent significant revenue that’s dangerously close to becoming a write-off.
- Low-Dollar, High-Volume Denials: Don't ignore these. Look for the patterns. Is one payer constantly denying the same low-cost service? Fixing that one systemic issue could recover thousands of dollars over the year.
This tiered method is a core principle of effective accounts receivable (AR) management and ensures you’re not wasting time on claims that won't move the needle.
Pro Tip: Give your team simple scripts for payer calls. Each script should outline the key info needed—claim number, patient ID, the specific denial reason—and end with a clear question: "What are the exact steps we need to take to resolve this?" This makes calls faster, less frustrating, and way more productive.
Use a ClearView Dashboard for Strategic Insight
To really get this process humming, you have to see your data clearly. A "ClearView Dashboard" isn't a specific brand of software; it's a concept. It’s a simple, at-a-glance report that shows you exactly where your money is getting stuck.
This dashboard should track a few vital signs for your practice's financial health:
- Denial Rate by Payer: Which insurance company is giving you the most grief?
- Denial Rate by Procedure Code: Are certain services consistently getting rejected?
- Days in AR: How long is it really taking you to get paid?
- Appeal Success Rate: Are your appeals actually working?
One of the biggest drivers of denials continues to be prior authorization. The good news is that the landscape is finally changing. By 2026, the widespread adoption of electronic prior authorization (ePA) systems is expected to slash approval times from weeks down to just minutes for many procedures. This is a critical shift, as payers are only getting stricter. Mastering ePA systems is non-negotiable for specialties like ENT and podiatry to keep pre-service denials from killing their cash flow.
Using Technology and Defining Clear Team Roles
You can’t just tweak workflows and hope your medical billing process improves. Real change happens when you empower your team with the right tools and give them crystal-clear responsibilities. This is the operational backbone of your entire revenue cycle.
When your tech and your talent are perfectly aligned, you build a system that isn’t just efficient—it’s resilient.
The funny thing is, many practices are already sitting on powerful tools that are just collecting dust inside their Electronic Health Record (EHR) software. Unlocking these features is often the lowest-hanging fruit for a quick and significant boost. This isn’t about buying something new; it’s about moving beyond basic scheduling to activate things like automated eligibility checks, electronic remittance advice (ERA) posting, and integrated claim scrubbers. These tools were literally designed to catch mistakes and get you paid faster.
Maximize Your Existing EHR and Billing Software
Before you even think about shopping for a new platform, do a deep dive into what you're already paying for. Your current system almost certainly has features that could make an immediate impact on your bottom line.
Get focused on mastering these three areas:
- Automated Eligibility Checks: This one is a no-brainer. Configure your system to run an insurance verification check the moment an appointment is booked and then again 24 hours before the visit. This simple automation prevents one of the absolute most common denial reasons: inactive coverage.
- Electronic Remittance Advice (ERA) Posting: If your team is still manually posting payments from paper EOBs, you're lighting dozens of hours on fire every single month. Setting up ERA allows payments to be posted automatically, freeing up your staff to work on high-value tasks like chasing down tricky denials and figuring out why they happened in the first place.
- Integrated Claim Scrubbing: Most modern systems have a built-in "scrubber" that acts as a quality check, flagging claims for common errors against payer rules before you hit submit. Turn this feature on. Train your team to resolve every single flag. It’s your first and best line of defense against preventable rejections.
Technology should reduce the administrative burden, not add to it. The entire goal is to automate the predictable stuff so your expert team can manage the exceptions.
Of course, all of this has to sit on a secure, HIPAA-compliant foundation. That part is non-negotiable. Protecting patient data isn’t just a box to check for regulators; it’s fundamental to maintaining patient trust and avoiding the kind of financial penalties that can shut a practice down.
Defining Roles for a High-Performing Billing Team
A well-trained team where every single person knows their exact role is your single most valuable asset. Ambiguity is the enemy—it breeds errors, creates accountability gaps, and kills morale. When roles are clearly defined, your team operates like a finely tuned machine, with smooth handoffs and a shared sense of ownership over the practice's financial health.
Take a look at how a simple structure can create clear swim lanes for your team, ensuring nothing falls through the cracks.
Essential RCM Roles and Key Responsibilities
Here’s a breakdown of the key players in your revenue cycle. When each person owns their role and understands their critical KPI, the whole system works better.
| Role | Primary Responsibility | Critical KPI |
|---|---|---|
| Front Desk / Patient Intake | Accurate demographic and insurance data capture; real-time eligibility verification. | Point-of-Service Collections Rate |
| Biller / Coder | Accurate coding, clean claim submission, and proactive denial follow-up. | Clean Claim Rate (>95%) |
| AR Specialist | Manages aging accounts, works complex denials, and handles payer appeals. | Days in AR (<35) |
| Credentialing Coordinator | Ensures all providers are correctly enrolled and re-attested with payers. | Zero Credentialing-Related Denials |
This structure creates clarity, but it only works if you commit to ongoing training. Regular sessions on payer updates, new coding guidelines, and software features aren’t optional—they’re essential. A team that truly understands how their individual tasks directly impact revenue is a motivated and effective one.
And finally, never, ever underestimate the importance of provider credentialing. It’s a quiet but deadly cause of claim rejections. A single lapse in a provider’s enrollment with a major payer can halt payments for weeks or even months. Designating one person as the credentialing coordinator to manage applications and track re-attestation deadlines is one of the simplest ways to protect a massive chunk of your revenue.
Tracking Success with the Right Performance Metrics
To truly get your billing process dialed in, you have to move from guesswork to a data-driven strategy. It’s an old saying, but it’s true: you can’t fix what you can’t see.
The final piece of the puzzle is establishing and consistently tracking the right Key Performance Indicators (KPIs). This is what turns your billing data from a pile of numbers into a clear story about your practice’s financial health. This isn’t about just glancing at a monthly collections report; it’s about digging into the metrics that reveal the real efficiency of your revenue cycle.
Core Metrics for Financial Clarity
To start, focus on a handful of high-impact KPIs. These numbers give you an objective look at where your process is humming along and where it needs immediate attention.
-
Clean Claim Rate (CCR): This is the gold standard. It measures the percentage of claims paid on the very first submission. Your goal should be 95% or higher. Anything less is a direct signal that something is broken in your front-end or coding workflows.
-
Days in Accounts Receivable (AR): This KPI tells you the average number of days it takes to actually get paid. A healthy practice keeps this number under 35 days. If you see this number start creeping up, it’s a clear sign your follow-up and denial management processes are losing steam.
Don’t just track the overall Days in AR. Break it down by payer. A high number for one specific insurance company might point to a contract issue or a systemic problem with how you submit claims to them. It’s often one or two payers dragging down the average.
Advanced KPIs for Strategic Insights
Once you’ve got the basics down, you can unlock much deeper, more powerful insights. These advanced metrics help you pinpoint the exact root causes of revenue leaks, not just the symptoms.
For a deeper dive, check out our complete guide on revenue cycle management best practices.
-
Denial Rate by Reason Code: Don’t just track that you have denials. Categorize every single one. Are most of your denials coming from simple registration errors? A lack of medical necessity documentation? Or sloppy coding mistakes? This data tells you precisely which part of your team needs more training or which process needs a complete overhaul.
-
Net Collection Rate (NCR): This is the ultimate measure of your billing effectiveness. It shows the percentage of the total potential reimbursement you actually collect from payers after all the adjustments. This KPI reveals exactly how much money you are leaving on the table from uncollected balances or contractual write-offs. It’s your financial reality check.
Got Questions About Medical Billing? We’ve Got Answers.
Running a practice means you’re constantly juggling patient care and the financial health of your business. It’s only natural that a few key questions pop up again and again as leaders try to get a handle on their revenue cycle.
Here are the straightforward, no-fluff answers to the questions we hear most often.
What’s the Single Most Impactful Thing a Small Practice Can Do?
For a small or solo practice, forget the complex workflows for a moment. The one change that delivers the biggest punch is mastering real-time insurance eligibility and benefits verification.
Seriously. This single front-end process prevents the vast majority of cheap, frustrating, and entirely avoidable denials. Get this right, and everything else gets easier.
Build a strict protocol: your team verifies coverage when the appointment is booked, and then they check it again 24-48 hours before the visit. This isn’t just about confirming a policy is active; it’s about clarifying the patient’s real financial responsibility. Do that, and you’ll sidestep countless downstream headaches and watch your clean claim rate climb.
How Often Should We Be Looking at Our Billing Performance?
Think of it like a clinical check-up for your revenue. You need to review your key performance indicators (KPIs) monthly. This cadence hits the sweet spot—it’s frequent enough to catch a negative trend before it turns into a cash flow crisis, but it gives you enough time to gather meaningful data.
Your monthly review should be a non-negotiable meeting that covers the vitals:
- Clean Claim Rate
- Days in Accounts Receivable (AR)
- Denial Rate (and you need to break this down by reason and payer!)
- Net Collection Rate
This simple rhythm transforms billing from a mysterious back-office task into a strategic lever for managing your practice.
A monthly KPI review is the financial equivalent of a clinical follow-up. It’s where you check the vital signs of your revenue cycle, diagnose what’s wrong, and adjust the treatment plan before things get worse.
When Is It Actually Time to Outsource Our Billing?
Deciding to outsource isn’t about throwing in the towel; it’s a strategic move. The writing is usually on the wall long before a practice owner makes the call.
It’s time to seriously explore your options when you see these warning signs:
- Your denial rate is consistently creeping above 10%.
- Your Days in AR are stretching past the 45-day mark.
- Your team is so buried in day-to-day tasks that working aging claims and fighting appeals feels impossible.
Outsourcing gives you immediate access to specialized expertise and technology without the massive overhead of hiring, training, and managing more staff. More importantly, it lets your team get back to focusing on patient care while dedicated experts work on one thing: getting you paid what you’ve earned.
Ready to stop revenue leaks and gain real financial clarity? The ClaiMed Solutions TrustedRCM Method combines pre-submission audits, a live ClearView Dashboard, and expert support to reduce denials and get you paid faster. Schedule your complimentary assessment today.